Why Showing Up Is Costing You More Than Calling In
You made it to the 9 a.m. call. You said the right things. But for about 40 minutes in the middle, you weren’t really there—you were managing a heat wave behind your sternum, trying to remember the word for what you were describing, hoping no one noticed the pause.
You showed up. You got nothing done. And next quarter, your performance review will not mention any of this.
Here’s the part nobody says out loud: being physically present while cognitively absent is draining your career and your earnings—quietly, consistently, and in ways that don’t show up on a sick day report.
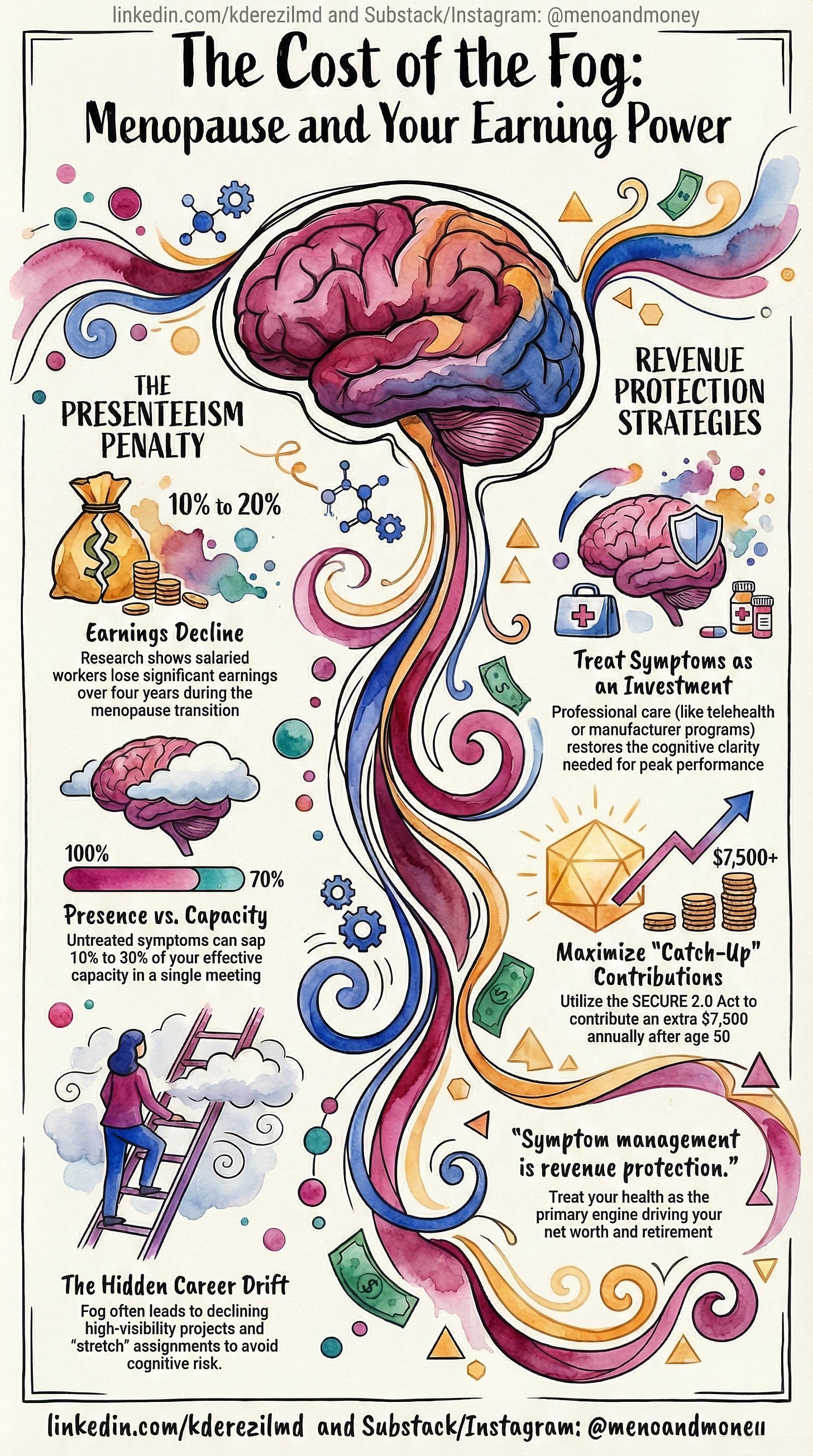
Presenteeism—showing up while symptomatic—is harder to measure than absenteeism, which is exactly why it goes unnamed. You don’t lose a day. You lose 10%, 20%, sometimes 30% of your effective capacity in a single meeting. Multiply that across weeks and months, and the financial shape of it becomes undeniable.
Myth: Taking time off is the risk. Reality: Staying foggy is.
Most women in perimenopause push through. The cultural instruction is clear: be present, be capable, don’t make it anyone else’s problem. So you show up—sleep-deprived, mid-flash, mid-sentence—and perform a version of your best work.
What’s true right now is that untreated menopause symptoms have been linked to measurable losses in career earnings. Research tracking women through the menopause transition found earnings can decline by roughly 10% over four years—with salaried workers losing closer to 20%, and self-employed women losing more. These aren’t abstract numbers. They are missed bonuses, stalled negotiations, and high-visibility projects quietly handed to someone else.
“Presenteeism doesn’t look like failure. It looks like showing up.”
The presenteeism penalty shows up across three categories:
Productivity costs: Avoiding the complex project. Letting someone else take the lead call. Not raising your hand for the stretch assignment—because you’re not sure your brain will cooperate.
Career drift: Declining speaking opportunities, mentorship roles, or cross-functional visibility—not from disinterest, but from a quiet calculation about cognitive risk.
Compounding retirement loss: Every year of flat or reduced income during your peak earning decade shrinks the base from which your retirement contributions—and Social Security benefit calculations—are made.
This doesn’t mean you’re failing. It means untreated symptoms have a cost that your employer isn’t tracking—but your net worth is.
“Symptom management isn’t self-care. It’s revenue protection.”
3 moves that protect what you’ve built
1. Make symptom care automatic, not optional Scheduling a telehealth appointment with a menopause-trained provider require no referral, no waiting room. Treated symptoms are not a luxury. They are an investment in your earning capacity. If cost is a barrier, GoodRx and manufacturer assistance programs can reduce or eliminate prescription costs.
2. Protect future you: check your beneficiaries today Log in to one retirement account this week—just one. Confirm the beneficiary designation is current. Not next month. Tonight, if you have five minutes. This is the lowest-effort, highest-stakes financial action on your list.
3. Automate the savings increase you keep meaning to make If your income has dipped or plateaued, increase your retirement contribution by even 1% this month—before your brain negotiates you out of it. The SECURE 2.0 Act now allows catch-up contributions of up to $7,500 per year after age 50. Use it. Future you is counting on present you to act before the fog rolls back in.
You don’t have to solve this tonight.
But if today felt like 60% of you showed up—that’s information, not failure. It’s the symptom talking. And the symptom has a treatment.
Reply with one word: ‘Foggy’ or ‘Fighting.’ I read every one.
And if this landed—forward it to the woman who keeps saying she can’t think lately. She’s not alone, and she deserves to know it.